Corneal tissue response to cross-linking treatment. Application to keratoconus treatment.
FUND AGENCY
Spanish Ministry of Research and Innovation through the research project DPI2014-54981R |
 |
SUMMARY
The human cornea provides more than two thirds of the optical power depending on the curvature, the regularity, the transparency and the refractive index.The corneal shape also depends on the equilibrium between its structural stiffness (related to the topography, pachymetry or thickness and the corneal tissue properties) and the applied forces such as the intra ocular pressure (IOP) and the external actions over the anterior corneal surface. Many of the diagnosis techniques to evaluate corneal tissue instabilities (ectasia) before or after refractive surgery (LASIK, PRK, SMILE, etc.) are based on registering the topography, measuring the IOP and on the pachymetry. Recently (2005 and 2010), two non-contact tonometers appeared on the market in order to study the corneal stiffness or stability. Nevertheless, none of them is able to evaluate the contribution of the tissue microstructure to the cornea stiffness. The objective of this project is to evaluate the mechanical behaviour of the tissue, uncoupling the effects of the geometry and the IOP. Therefore, it will be necessary to combine diagnosis techniques (non contact tonometry) on corneas of an animal model, with personalized finite element models of the eyeball. By using inverse analysis and optimization techniques, the mechanical properties that reproduce the experimental results will be determined.
Determining in vivo mechanical properties of the corneal tissue will allow studying the efficiency of the crosslinking treatment. This is mainly used for stopping the apparition or progression of biomechanical instabilities of the corneal stroma (corneal ectasias, keratoconus, induced by surgery or infectious keratitis). Thus, an animal model (New Zealand white rabbit) will be used and morphological and mechanical changes will be evaluated depending on the used technique (UVA power, the exposure time, riboflavin type, etc.).
RESULTS
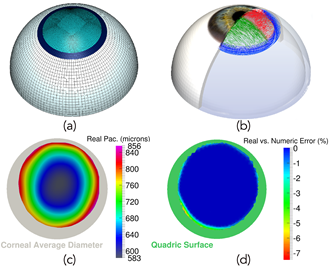
Patient–specific corneal geometry |
|
MAIN PUBLICATIONS:
- A. Ariza-Gracia, David P. Piñero, J. Zurita, José F. Rodriguez, B. Calvo. Coupled Biomechanical Response of the Cornea Assessed by Non-Contact Tonometry. A simulation study. Plos One, 10(3), pp:1-15, 2015 . DOI: 10.1371/journal.pone.0121486
- A. Ariza-Gracia, David P. Piñero, José F. Rodriguez, Rafael J. Pérez-Cambrodí, B. Calvo. Preliminary evidence of the interaction between diurnal variations of intraocular pressure, pachymetry and corneal response to an air-puff. JCRS Online Case Reports, 3 (1), 12-15, 2015. DOI: 10.1016/j.jcro.2015.01.002
- A. del Buey, E. Lanchares, J.A. Cristóbal, S. Ramón y Cajal, C. Yus, B. Calvo. Immediate effect of the ultraviolet-A collagen cross-linking therapy on the biomechanics and histology of the human cornea. Journal of Refractive Surgery, 2015, 31. 1, pp: 70-71. DOI: 0.3928/1081597X-20141218-08
- Del Buey, M.A., Lanchares, E., Calvo, B., Lavilla, L., Almenara, C., Pérez, I., Idoate, A., Pinilla, I., Ascaso, J. and Cristobal, J. Immediate Effect of Ultraviolet-A Collagen CXL Therapy on Biomechanics and Histology of Human Cornea. Acta Ophthalmologica, 93: n/a. doi: 10.1111/j.1755-3768.2015.0576, 2015
- A. Ariza-Gracia, J. Zurita, David P. Piñero, B. Calvo, José F. Rodriguez. Automatized Patient-Specific Methodology for Numerical Determination of Biomechanical Corneal Response. Annals of Biomedical Engineering, 44(5), pp: 1753-72, 2016. DOI: 10.1007/s10439-015-1426-0
- Lanchares, M.A. del Buey J.A. Cristóbal, B. Calvo J. Ascaso and M.Malve. Computational simulation of scleral buckling surgery for rhegmatogenous retinal detachment: on the effect of the band size on the myopization. Journal of Ophthalmology, Article ID 3578617, 10 pages, 2016. doi:10.1155/2016/3578617
- A. Ariza-Gracia, S. Redonde, David P. Piñero , B. Calvo , José F. Rodríguez. A predictive tool for determining patient specific mechanical properties of human corneal tissue. Computer Methods in Applied Mechanics and Engineering, 317, pp. 226 – 24, 2017. DOI: 10.1016/J.cma.216.12.013
- Ortillés, P. Goñi, E. Rubio, M. Sierra, E. Gámez, M. T. Fernández, M. Benito, J. A. Cristóbal, B. Calvo. A rabbit model of Acanthamoeba keratitis: use of infected soft contact lenses after corneal epithelium debridement with a diamond burr . Investigative Ophthalmology & Visual Science, 58:1218–1227, 2017. DOI:10.1167/ iovs.16-21100
- Ortillés, J.F. Rodriguez, M. A. Ariza-Gracia, G. Pascual, B. Calvo. Why non-contact tonometry tests cannot evaluate the effects of corneal collagen crosslinking.Journal of Refractive Surgery; 33(3):184-192, 2017
- Ortillés E. Rubio, M. T. Fernández, M. Benito, J. A. Cristóbal, B. Calvo , P. Goñi. In vitro development of an effective treatment of Acanthamoeba keratitis. International Journal of Antimicrobial Agents, In press, 2017
- Ortillés E. Lanchares, J. A. Cristóbal, B. Calvo. Use of 2% hydroxypropyl methylcellulose to prevent the corneal swelling during the in vitro mechanical characterization. Journal of Materials: Design and Applications. In press, 2017
- A. Ariza-Gracia, A. Ortillés, J. A. Cristóbal, José F. Rodríguez, B. Calvo. A numerical-experimental protocol to characterize corneal tissue with an application to predict astigmatic keratotomy surgery. Journal of the Mechanical Behavior of Biomedical Materials, In press, 2017.DOI: 10.1016/j.jmbbm.2017.06.017